Upper Tract Urothelial Cancer
Less than 5% of kidney cancers arise from the lining of the kidney (renal pelvis) or ureter. These cancers are called upper tract urothelial cancers or transitional cell carcinomas. The cells that line the kidneys and ureter are the same as those that line the inside of the bladder, as such these cancers are similar to bladder cancers. The main risk factor for developing upper tract urothelial cancer is smoking.
Upper tract urothelial cancers most commonly cause blood in the urine (haematuria). They can if they grow large enough block the flow of urine from the kidney and cause pain in the back/loin. Some cancers are picked up by chance in the investigation or follow up of patients with bladder cancer
Investigation
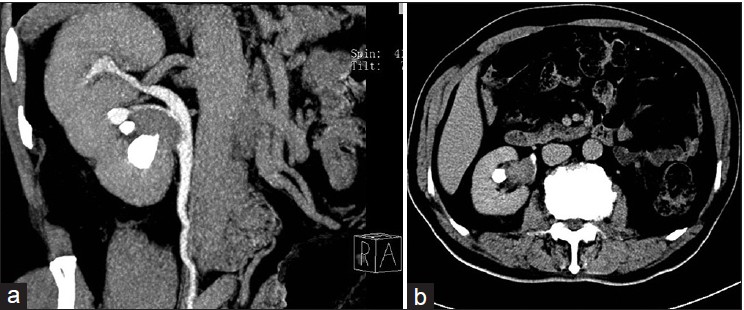
CT urography is the best way of investigating the kidneys for upper tract urothelial cancers. This special CT scan involves giving an injection of contrast into the vein and performing numerous scans of the kidneys at different time point.
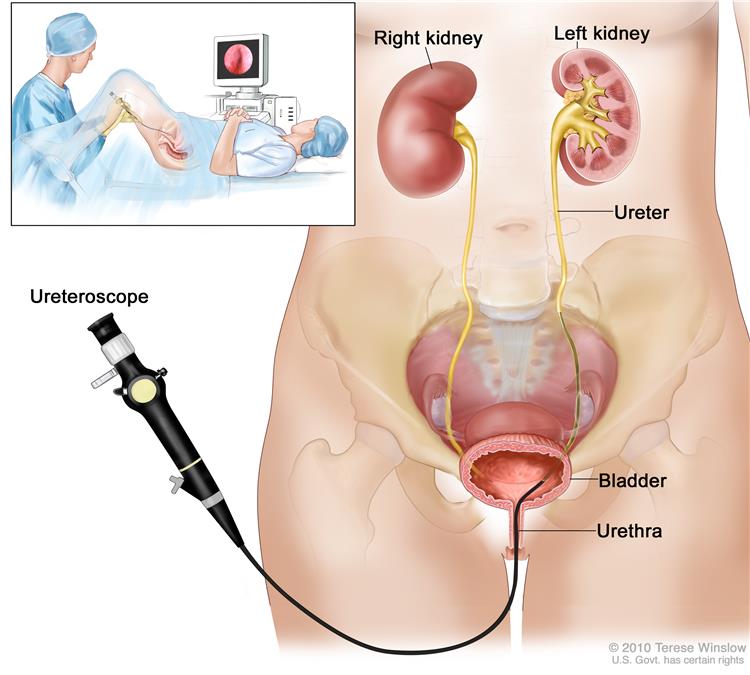
If a CT scan suggests a urothelial cancer in the ureter or renal pelvis then patients are advised to have a diagnostic uretero-renoscopy and biopsy. This is an procedure involved passing a telescope into the ureter and kidney to directly inspect the inside of the urinary system for potential cancers. Any abnormal areas are biopsied to allow the pathologist to confirm the diagnosis. Patients with a suspected upper tract urothelial cancer should have a staging CT scan of the Chest and Abdomen to look for any disease spread.
Treatment
The standard treatment for patients with an upper tract urothelial cancer is a radical nephroureterectomy. This operation involves the complete removal of the kidney and ureter all the way down to the bladder. This is usually done as a laparoscopic procedure and involves a 5 day stay in hospital.
In some patients these cancers can successfully managed with a laser ablation. In this operation a flexible telescope is passed up the ureter to the tumour and the cancerous area destroyed with a laser beam.